Atherosclerosis and stroke are closely related because they share common risk factors. In fact, having atherosclerosis can increase the risk of experiencing a stroke. By proactively managing the risk factors that cause atherosclerosis, individuals can significantly reduce their stroke risk and prevent other complications.
Even if you have already experienced a stroke, managing or preventing atherosclerosis is still important for your recovery journey. By monitoring this, you can reduce your risk of additional strokes and maximize your outcome. To help you understand the relationship between atherosclerosis and stroke, this article will discuss:
- The relationship between atherosclerosis and stroke
- Risk factors for atherosclerosis and stroke
- Signs of a stroke due to atherosclerosis
- How to manage atherosclerosis to prevent a stroke
The Relationship Between Atherosclerosis and Stroke
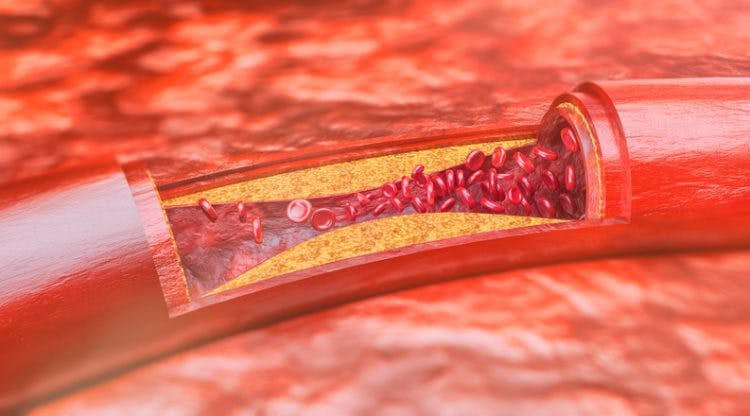
Atherosclerosis develops when blood cells, fat, cholesterol, and other substances accumulate in the inner lining of your arteries. This buildup is called plaque and it can cause the arteries to narrow and harden. As arteries become narrower due to plaque buildup, blood flow to other areas of the body becomes gradually obstructed. According to the NIH, around half of Americans between ages 45 and 84 have atherosclerosis.
Now, let’s discuss how atherosclerosis is related to stroke. In short, a stroke takes place when the brain’s blood flow is compromised. This leads to cell death and tissue damage within the brain. A stroke can be caused when an artery within or leading to the brain becomes blocked (ischemic stroke) or bursts (hemorrhagic stroke). This impairs the supply of oxygen-rich blood to the brain and causes the affected areas to lose their important functions.
Atherosclerosis can affect the arteries in any region of the body. This includes the arteries leading to the brain, called the carotid and vertebral arteries, or arteries within the brain, known as the intracranial arteries. When atherosclerosis causes these arteries to narrow, it increases the risk of an ischemic stroke. In fact, most ischemic strokes are caused by atherosclerosis.
Ischemic strokes can be caused by atherosclerosis via two main mechanisms. One is the gradual narrowing of the artery due to plaque buildup. When the artery feeding the brain becomes mostly or completely blocked, blood flow is impaired and a stroke takes place. Another mechanism is the creation of an embolism. In these cases, a plaque in another area of the body may break and form a clot. When this clot travels to the brain and lodges itself in an artery, a stroke can follow. This is why managing risk factors for atherosclerosis is vital.
Risk Factors for Atherosclerosis and Stroke
While atherosclerosis and stroke are two different medical conditions, these are closely related and share many of the same risk factors. Educating yourself on these shared risk factors can help you reduce your risk of atherosclerosis and, therefore, stroke.
Common risk factors for both atherosclerosis and stroke include:
- High cholesterol
- High blood pressure (hypertension)
- Smoking
- Poor diet
- Diabetes
- Obesity
- Insufficient physical activity
- Increased age
- Family history of heart disease
Many of these risk factors contribute to the buildup of plaque within the arteries and increase the chances of blood clotting or artery blockage. For example, smoking causes blood vessels to further constrict and limits blood flow. Similarly, uncontrolled high blood pressure can damage the walls of arteries that have been narrowed by plaque buildup.
While you may not be able to control factors like age or family history, you can still decrease your risk by practicing healthy habits and having regular appointments with your primary care provider. By effectively managing these risk factors, individuals can significantly minimize their risk of developing atherosclerosis and having a stroke. Before we talk about management tips, let’s review the signs of a stroke and when to seek emergency medical care.
Signs of a Stroke Due to Atherosclerosis
Individuals with atherosclerosis often do not experience symptoms until the condition becomes severe. As a result, many people do not get diagnosed with atherosclerosis until after they have a stroke. When a blood clot gets caught in a narrowed artery, the supply of oxygen-rich blood to the associated area of the brain gets cut off. As a result, individuals may experience the sudden onset of stroke warning signs, which we will review now.
Stroke Warning Signs
- Weakness or paralysis of a limb or side of the body
- Facial drooping
- Confusion
- Speech difficulties such as slurred words
- Vision problems
- Dizziness
- Sudden, severe headache
- Vertigo
If you notice yourself or anyone around you experiencing any of these signs, seek emergency medical attention immediately. Timing plays an essential role in the treatment of a stroke. For example, a blood-thinning drug called tPA may be used to clear the blood clot and restore blood flow within 3 hours of symptom onset. Timely treatment can help minimize damage to the brain and preserve as much function as possible.
We’ve talked about how atherosclerosis leads to stroke, but it’s important to note that this condition can also lead to complications in other areas of the body. For example, atherosclerosis can cause symptoms such as:
- Chest pain or angina
- Leg pain with activity
- Shortness of breath
- Nausea
- Stomach pain after eating
- Extreme fatigue
While these symptoms may not be associated with stroke, they are often equally as serious. When possible, it’s best to be proactive and manage atherosclerosis before a stroke or other complication happens. We will now discuss the various ways you can manage atherosclerosis to help you prevent a stroke altogether.
How to Manage Atherosclerosis and Prevent Stroke
Treatments for atherosclerosis typically focus on minimizing the formation of blood clots, reducing risk factors, and expanding the arteries. Various interventions such as adopting new healthy habits, taking medications, or even undergoing surgery may be recommended. Talk with your doctor to come up with the best plan that meets your unique needs.
Managing atherosclerosis sometimes requires a multi-sided approach. Depending on the severity of plaque buildup in your arteries, you may be able to manage atherosclerosis using conservative measures. However, some may require more intensive interventions. Let’s review some ways you can manage atherosclerosis to potentially prevent a stroke.
1. Making Healthy Lifestyle Changes
Adopting healthy lifestyle changes is one of the most effective ways to prevent atherosclerosis from progressing. You can establish many daily habits to maximize your health and reduce your stroke risk. Start small and continue to make these healthy changes to meet your wellness goals.
Quitting smoking can reduce your risk of atherosclerosis and stroke and is an important step in improving your overall health and wellness. Additionally, increasing your physical activity can improve your heart health and decrease both atherosclerosis and stroke risk. You can check out these physical activity guidelines to help you get started.
Following a heart-healthy diet plan and maintaining a healthy weight are other healthy habits you can use to minimize your risk of having a stroke. This is because prioritizing healthy foods can reduce plaque buildup in your arteries and help manage cholesterol. This booklet from the NIH is a great resource that guides you through lowering your cholesterol through diet and lifestyle changes.
2. Antiplatelet Medications
Antiplatelet medications thin the blood and discourage the formation of blood clots or plaques. Common antiplatelet medications include clopidogrel (Plavix), prasugrel (Effient), and acetylsalicylic acid (Aspirin). Aspirin can help prevent stroke when atherosclerosis is present. However, always consult your doctor before taking daily aspirin to make sure it’s safe. In some individuals, such as those with high blood pressure, daily aspirin can cause more harm than good.
If your doctor prescribes you any of these medications, it’s essential to be extra careful and pay attention to any skin tears or wounds, no matter how small. Your body may not be able to clot as fast to stop the bleeding because of the antiplatelet medication.
3. Statin Medications
Statins are medications that help lower your LDL cholesterol levels. You may hear LDL cholesterol referred to as ‘bad’ cholesterol. This is because LDL cholesterol contributes to the buildup of plaque in your arteries and promotes atherosclerosis. Reducing LDL cholesterol levels can significantly minimize the progression of atherosclerosis and potentially reverse plaque buildup in the arteries.
It is important to work closely with your doctor to determine the right medication for your needs and symptoms. Always follow the instructions given with your prescription and never stop taking a medication without consulting your doctor first. They will be able to help explain risk factors and make modifications to your medication if necessary.
4. Angioplasty and Stenting
Angioplasty and stenting are surgical procedures that expand arteries narrowed by plaque buildup. These surgeries can be performed on the arteries in the neck leading to the brain (carotid or vertebral arteries) or the arteries within the brain (the intracranial arteries).
Angioplasty involves placing a thin catheter into a narrowed artery. Once it is properly positioned, a tiny balloon at the end of the catheter is inflated to widen the artery and restore normal blood flow. Then, stenting is performed, which involves placing a small tube (a stent) into the artery to keep it expanded long-term. Intracranial angioplasty is an effective method of stroke prevention for those at high risk.
5. Cerebral Artery Bypass Surgery
During cerebral artery bypass surgery, a surgeon will reroute blood flow around an atherosclerotic artery to prevent a blood clot from getting stuck and causing stroke. This surgery is generally preferred over an angioplasty and stent placement when there is severe atherosclerosis of the artery.
There are 2 ways to perform a cerebral artery bypass surgery. The first method involves taking an artery or vein from elsewhere in the body, called a vessel graft. The surgeon then connects the vessel both above and below the blocked artery to reroute blood flow. The second method involves detaching one end of an artery already present in the scalp or face, called a donor artery, and connecting it to an artery on the surface of the brain. This donor artery becomes the new blood flow source to this brain region.
6. Carotid Endarterectomy
The carotid arteries are the primary suppliers of blood to the brain. When atherosclerosis develops in these arteries, individuals are at major risk for a stroke. To help prevent a stroke, a surgeon can perform a carotid endarterectomy, which involves going directly into the carotid artery and removing excess plaque.
As you can see, there are many surgical options to help manage atherosclerosis and prevent stroke. While the surgeries we’ve reviewed are some of the most common, every person is unique and may require different interventions. By working closely with your doctor, you will be able to create a personalized treatment plan. Remember, even if surgery is necessary, it is still important to make healthy lifestyle changes to maximize your results.
Atherosclerosis and Stroke: Key Points
Atherosclerosis and stroke are closely related and share many risk factors. Excess plaque in the arteries caused by atherosclerosis can affect the brain’s blood supply. This can lead to an ischemic stroke and cause tissue damage within the brain. For this reason, it is important to manage your risk factors and prevent a stroke from taking place.
There are several ways to manage atherosclerosis before it leads to a stroke. Making healthy lifestyle changes can reduce plaque buildup and decrease the narrowing of the arteries. These healthy changes include quitting smoking, increasing physical activity, and prioritizing a healthy diet.
For some, lifestyle changes alone may not be enough to curb atherosclerosis and reduce stroke risk. Medications such as antiplatelets and statins can reduce clotting or help manage LDL cholesterol. Furthermore, some individuals may need to pursue surgical interventions to bypass or clear arteries affected by atherosclerosis.
If you or a loved one have atherosclerosis and worry that it may lead to a stroke, now is the time to talk to your doctor for recommendations. They can provide you with treatment options to increase your health and help prevent a stroke. Keep making small daily changes to optimize your wellness and make health a lifestyle.