Autonomic dysfunction is one of the many possible side effects of a concussion. It occurs due to damage of the autonomic nervous system.
Unfortunately, most people with autonomic dysfunction do not recognize its symptoms, and therefore live with it for years without seeking treatment.
To help you better understand this problem, you’re about to learn the causes and symptoms of autonomic dysfunction after concussion.
Use the following links to jump ahead to the relevant section:
- What is the Autonomic Nervous System?
- Causes of Autonomic Dysfunction After Concussion
- Symptoms of Autonomic Dysfunction After Concussion
- Diagnosing Autonomic Dysfunction
- Treating Autonomic Dysfunction After Brain Injury
What is the Autonomic Nervous System?
Autonomic dysfunction (also called dysautonomia) refers to a dysfunction of the autonomic nervous system (ANS).
The autonomic nervous system is a network involving the amygdala, hypothalamus, and brain stem, among other areas int he brain. It controls all involuntary bodily functions, such as:
- Blood vessel dilation or constriction
- Heart rate
- Blood pressure
- Digestion
- Adrenal gland function
- Thermoregulation (regulating body temp)
In addition, the ANS has two distinct branches, called the sympathetic and parasympathetic nervous systems, each with its own purpose.
Causes of Autonomic Dysfunction After Concussion
The two branches of the autonomic nervous system have separate but critical functions:
- Sympathetic nervous system (SNS). This branch controls the body’s “fight or flight” response. When the sympathetic nervous system activates, your body releases adrenaline, which triggers a cascade of responses such as increased heart rate and rapid breathing.
- Parasympathetic nervous system (PNS). This response counters the sympathetic response by decreasing the body’s response to adrenaline while lowering heart rate and blood pressure.
The parasympathetic system connects to the rest of the body through a cluster of cranial nerves at the base of the skull. Therefore, it is vulnerable to damage after a concussion or mild traumatic brain injury, which can lead to autonomic dysfunction.
If an injury affects these nerves, the parasympathetic nervous system cannot respond appropriately. As a result, the SNS will continue to put the body into a constant state of distress. This is known as sympathetic dominance and means the SNS is more in control than it should be.
If the brain injury was severe, the sympathetic response will be strong and will flood the body with adrenaline and other hormones. If this goes on too long, autonomic dysfunction can occur.
Symptoms of Autonomic Dysfunction After Concussion

In the past, autonomic dysfunction was thought to only occur after severe brain injuries. However, recent studies have shown that ANS problems are a common and “previously unrecognized cause of dizziness following concussions.”
Autonomic dysfunction after concussion can cause serious side effects. Some of these include symptoms such as:
- Decreased immune system
- Dizziness and fainting upon standing up
- High or low blood pressure
- Light sensitivity
- Hyperhidrosis (excessive sweating)
- Digestive problems
- Cold or heat sensitivity
Depending on how much of your ANS was affected after your concussion, you can experience one or all of these symptoms. In addition, their effects can range from mild to severe.
In addition, autonomic dysfunction, if left untreated for too long, can cause cardiac problems, including arrhythmias, arterial blockage, and heart failure.
Therefore, it’s crucial to diagnose and treat autonomic dysfunction as soon as possible.
Diagnosing Autonomic Dysfunction
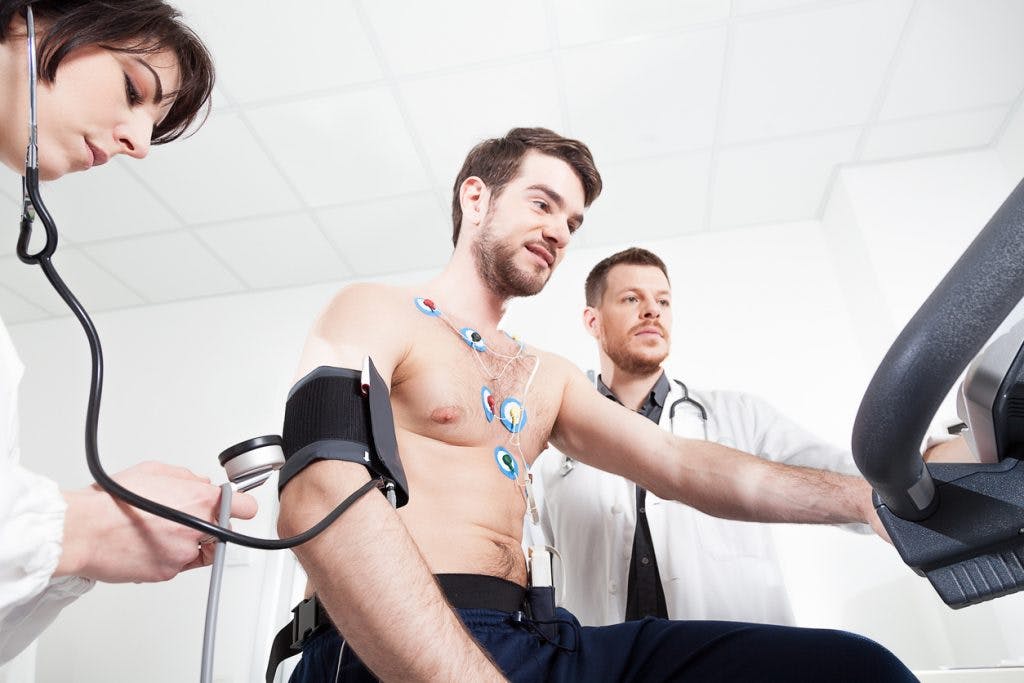
The best way to diagnose autonomic dysfunction is by measuring heart rate variability (HRV).
To do this, a doctor will give the patient a Holter monitor that records heart function for 24 hours. A Holter monitor is a noninvasive device attached to your chest via electrodes, which allows you to continue with normal daily activities.
Recording your heart function can help doctors see whether your parasympathetic symptom is functioning properly. For example, in healthy persons, there will be continuous variations in heart rate, sometimes slightly elevated, sometimes low. This indicates that the ANS is functioning well and keeping the body regulated.
If autonomic dysfunction is present, however, the heart rate will not show as much variation. It will either be consistently high or low. That’s because there is no longer any back and forth between the sympathetic and parasympathetic responses.
Other methods for diagnosing autonomic dysfunction after a concussion include tests such as a pupillary light reflex test and graded exercise testing.
Treating Autonomic Dysfunction
In the vast majority of cases, autonomic dysfunction will resolve once the brain recovers from its concussion and the nerve damage heals.
However, if symptoms persist or are too severe, the best approach is to treat the symptoms. For example, beta-blockers will help manage irregular heartbeats, and blood pressure meds can keep your blood pressure from getting too high or low. You can also manage low blood pressure by making certain lifestyle changes, such as:
- Elevating the head of your bed
- Adding salt to your diet
- Drinking enough fluids
- Wearing compression stockings to prevent blood from pooling in your legs
Some diet changes will also help regulate digestion issues if those are affecting you. In addition, certain natural remedies for post-concussion syndrome might be able to reduce your symptoms.
Finally, since symptoms of autonomic dysfunction can vary, it’s important to talk to your doctor. He or she can help you find the most effective treatment for your condition.
Understanding Autonomic Dysfunction After Concussion
Autonomic dysfunction typically occurs when a concussion damages the parasympathetic nerves. This can lead to several serious side effects such as dizziness, high blood pressure, and excessive sweating.
Since each person with autonomic dysfunction may display different symptoms, treatment can take many different forms. Therefore, it is crucial to consult with a neurologist before starting any specific therapies.