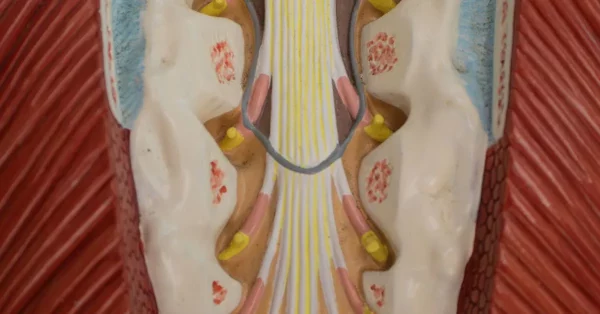
The spinal cord is a bundle of nerves that transmits messages between the brain and the rest of the body, including the muscles, organs, and peripheral nerves. Following a spinal cord injury, these signals may become disrupted, resulting in a loss of motor control and sensation. To preserve as much function as possible and prevent the progression of secondary damage, spinal cord surgery may be necessary.
To help you understand what spinal cord surgery entails, this article will guide you through:
- Types of spinal cord surgeries
- How timing of spinal cord surgery affects outcomes
- What to expect after spinal cord surgery
Types of Spinal Cord Surgeries
In the United States, a large percentage of individuals with spinal cord injury undergo surgery. Depending on the severity of the spinal cord injury, different types of spinal cord surgeries may be recommended.
Generally, the goals of spinal cord surgery are relatively straightforward. They include:
- Decompressing the spinal cord
- Stabilizing the spinal column (the vertebral bones and tissues surrounding the spinal cord)
These two types of surgeries will help to preserve as much neurological function as possible and prevent the progression of secondary damage. Below, we’ll discuss when each type of surgery is appropriate.
Decompression Surgery
It’s suggested that the most effective treatment for minimizing damage following spinal cord injury is early decompression surgery within 24 hours of injury.
Decompression surgery after spinal cord injury involves removing fragments of vertebrae or any foreign objects that are pressing down on the spinal cord. This helps minimize further tissue damage by relieving pressure off of the nerve roots and minimizing the progression of secondary damage such as inflammation, oxidative stress, and programmed cell deaths.
Commonly performed spinal cord decompression surgeries include:
- Laminotomy: removing a section from the back of the vertebra (the lamina)
- Laminectomy: removing the entire lamina
- Discectomy: removing a portion of a vertebral disc
- Foraminotomy or Foraminectomy: removing a relatively small or large amount of bone (respectively) to expand the nerve root openings
Your surgeon will determine the most appropriate type of decompression surgery based on the location and severity of your SCI.
Stabilization Surgery
Because the spinal column protects the spinal cord, stabilization is essential. It helps ensure that there are no loose particles that might later compress the spinal cord.
Surgery to stabilize the spine after spinal cord injury is called spinal fusion. It involves linking two or more vertebrae together with screws, rods, and bone grafts.
Over time, the bone grafts will promote bone production. This new bone growth will fuse the vertebrae together to stabilize the spinal column long-term.
Now that you understand the various surgeries that may be performed after a spinal cord injury, let’s discuss the controversy regarding the ideal timing of spinal cord surgery.
How Timing of Spinal Cord Surgery Affects Outcomes

The debate over the ideal timing for spinal cord injury surgery has been controversial.
The two conflicting views are that:
- The sooner decompression surgery is performed, the less overall damage will occur.
- Waiting a couple of days to perform surgery will allow the spinal cord to stabilize and be less reactive.
While more research is necessary to come up with a conclusive statement, it appears that more studies support earlier surgical intervention.
For example, this study compared the effects of early decompression surgery (within the first 8 hours after SCI) with later surgeries. After taking note of functional outcomes throughout the year following the surgery, the early decompression group showed better functional and recovery outcomes.
Ultimately, the timing of surgical management for spinal cord injury will vary case-by-case depending on the severity of the injury and the surgeon’s discretion. Up next, we’ll discuss what to expect after your spinal cord surgery.
What to Expect After Spinal Cord Surgery
After a spinal cord surgery, individuals may feel as if they’re in a completely different body due to loss of sensation and motor control. Rehabilitation after SCI focuses on reteaching the brain, muscles, peripheral nerves, and spinal cord to work in sync again through continuous repetition.
The spinal column can be extremely fragile after surgery, so individuals will likely need to wear a brace for structural support.
Once they are cleared by their physician, individuals should participate in physical and occupational therapy to learn how to adjust and maximize their mobility. Specialists in both types of rehabilitative therapies will evaluate the patient’s functional abilities and create a customized recovery plan.
Physical therapy will focus on developing gross motor function through targeted exercises. In contrast, occupational therapy will focus on improving mobility by practicing activities of daily living. If necessary, an occupational therapist may also teach you how to use adaptive tools to become more independent.
Additionally, your physician may also recommend participating in psychotherapy to help you cope with the emotional effects of life after spinal cord injury. There, you will learn how to effectively address changes in your mental health status, which may help put you in a better headspace for pursuing rehabilitation.
Because every SCI is unique, it’s ideal to seek personalized rehabilitation that caters to your specific lifestyle and concerns.
Understanding Spinal Cord Surgery: Key Points
Generally, spinal cord surgery focuses on decompression of the spinal cord and stabilization of the spine.
While surgery won’t reverse damage to the spinal cord, it can often minimize or prevent further damage from developing.
We hope this article helped you better understand what spinal cord surgery involves and what to expect as you recover.