Following a severe brain injury, individuals may experience major changes in their movements and cognitive abilities. This can lead to difficulties performing everyday activities independently as well as socializing. Fortunately, even after the most severe brain injuries, there is hope for recovery.
To help you navigate the road to recovery after severe brain injury, this article will discuss:
What is Considered a Severe Brain Injury?
While most brain injuries are mild, about 10-15% result in serious injuries that require more intensive care. A severe TBI is defined as a brain injury that results in a loss of consciousness longer than 6 hours, and a Glasgow Coma Scale score of 3 to 8 points.
The Glasgow Coma Scale assesses one’s motor functions, eye movements, and verbal responses to determine an individual’s level of cognitive function. The lower the final score, the more severe the traumatic brain injury.
After severe brain injury, most individuals pass through several levels of unconsciousness, including:
- Coma. The deepest state of unconsciousness. Patients in a coma are unresponsive to their environment and cannot wake up, even when stimulated.
- Vegetative State. Persons in a vegetative state may sometimes seem awake. But while their eyes can open and close, they have no awareness of their surroundings. Rather, these reactions are caused by autonomic responses.
- Minimally Conscious State. A patient in a minimally conscious state has recovered a reduced sense of awareness. They can sometimes follow very basic one-step instructions and react to stimulation (touch, sounds, light, etc.), but they will often dip back into unconsciousness.
The duration of a coma after brain injury primarily depends on the location and severity of the injury. Most individuals who sustain a severe brain injury remain unconscious for several weeks before they begin to regain consciousness. However, it’s also possible for individuals to remain in a coma for months before waking up. Generally, the sooner a person emerges from a coma, the better their chances of achieving a full recovery.
Once an individual emerges from a coma, they may experience various changes in sensation, movement, and cognition.
Effects of Severe Brain Damage
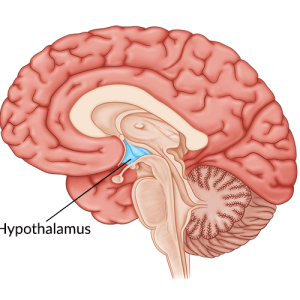
Depending on which area(s) of the brain are affected, severe brain injury can result in a wide range of secondary effects.
Some of the most common effects of severe brain damage include:
- Speech difficulties. Severe brain injury often leads to communication difficulties such as aphasia, which can cause problems with understanding and/or producing words.
- Swallowing problems. Another common effect of severe brain injury is difficulty swallowing, known as dysphagia.
- Sensory disorders. Severe brain injuries can cause several sensory disorders to occur. The most common sensory issues after TBI include hearing loss and numbness.
- Cognitive deficits. Damage to the frontal lobe often causes severe cognitive deficits, such as difficulties with attention, memory, and critical thinking.
- Vision problems. Vision is primarily processed in the visual cortex, which resides in the occipital lobe. If the visual cortex becomes damaged, visual problems such as partial blindness, double vision, or blurred vision can occur.
- Left neglect. Damage to the right hemisphere of the brain can lead to a condition known as left neglect. With left neglect, the person cannot detect objects or sounds that come from the left side of their environment.
- Changes in behavior. Severe brain injury may affect an individual’s impulse control, emotional regulation, and social skills.
- Muscle weakness. Depending on where the brain damage occurs, muscle weakness (or even paralysis) in the arms, legs, or trunk can occur.
- Balance problems. Whether due to muscular weakness in the trunk or legs, or some other cause (vision changes, damage to the vestibular system, etc.), balance issues are very common after severe brain injuries.
- Spasticity and contractures. Spasticity refers to involuntary muscle contractions caused by disrupted communication between the brain and the muscles. If left unmanaged, the muscle fibers can become permanently shortened, leading to contractures.
Fortunately, it is possible to treat most of these conditions by participating in various therapy techniques.
Want 20 pages of brain injury recovery tips in PDF form? Click here to download our free ebook “15 Things Every TBI Survivor Must Know” (link opens a pop up for uninterrupted reading)
Severe Brain Injury Recovery

Every brain injury is unique and results in different outcomes depending on the location and severity of the injury. Fortunately, because the brain has neuroplasticity, there is often hope for recovery even after the most severe TBIs.
Neuroplasticity refers to the brain’s ability to reorganize its neural circuitry to make adaptive changes. It allows for unaffected regions of the brain to learn and recover functions affected by brain damage.
The most effective way to promote neuroplasticity is to focus on consistency and repetition. When you repeatedly practice a function affected by brain injury, it stimulates the brain and reinforces demand for that function. This encourages the brain to utilize neuroplasticity to rewire itself. The more you practice, the stronger the newly rewired connections become.
Below are some examples of therapies that utilize neuroplasticity to boost recovery:
1. Physical Therapy
After a severe brain injury, individuals may experience paralysis or severe weakness. A physical therapist can guide individuals through targeted exercises to stimulate the brain and promote neuroplasticity.
If decreased motor control is affecting your ability to move your limbs on your own, a physical therapist may perform passive range of motion exercises. This involves moving the client’s paralyzed or severely weakened limb for them. Although they are not actively performing the movement, the movement itself still stimulates the brain and encourages neuroplasticity.
Eventually, with consistent and repetitive passive exercise, individuals may develop better control over their movements. At this point, a physical therapist may start having them perform more active exercise (where they are initiating the movement themselves, possibly with light assistance or supervision from the therapist), with goals of improving strength and balance and progressing towards walking.
Want 25 pages of TBI recovery exercises in PDF form? Click here to download our free TBI Rehab Exercise ebook now (link opens a pop up for uninterrupted reading)
2. Constraint-Induced Movement Therapy (CIMT)
Constraint-induced movement therapy is an intervention designed to prevent learned non-use after a severe brain injury. Learned non-use occurs when a person develops methods that help them avoid using their affected muscle.
For example, if a brain injury has made an individual’s right hand weaker, they might start to solely use their left hand to perform everyday tasks. Unfortunately, if this persists, the right hand will continue to weaken until it is effectively useless. Therapists refer to this as learned non-use.
CIMT attempts to thwart this process by forcing the individual to use their affected muscles. This typically involves constraining use of the unaffected limb by wearing an oven mitt or simply placing it behind the back. The hope is that by intensively using the affected arm, neuroplasticity will kick in and motor control over will improve.
3. Occupational Therapy
Occupational therapy can help individuals improve their functional independence after severe brain injury. This often involves practicing activities of daily living such as grooming, toileting, and feeding.
Occupational therapy prepares individuals to address the activities and tasks that occupy their everyday lives. Some areas of life an occupational therapist can help with include:
- Self-care
- Home management
- Recreation
- Social skills
- Cognitive functioning
- Returning to school/work
If motor or cognitive functions are severely affected, an occupational therapist can suggest compensatory techniques (such as setting reminders on a phone or using adaptive tools) to help the client become more independent.
4. Speech Therapy
If a severe brain injury causes cognitive deficits, aphasia, or other communication disorders, participation in speech therapy is essential. A speech therapist guides individuals through various speech therapy activities to help them retrain their brains and regain language skills.
In addition, a speech therapist can assess any cognitive skills that may be affected by injury. For example, individuals might need to work on their ability to listen, pay attention, and respond appropriately.
5. Sensory Re-Education
Sensory re-education, also known as sensory retraining, is a form of cognitive-behavioral therapy that helps the brain relearn how to process sensation again. It works by exposing individuals to different sensations and helping them learn how to distinguish between them again. The therapy has been proven effective at activating neuroplasticity and helping people regain feeling.
Most occupational therapists are familiar with sensory reeducation and can teach clients different types of sensory stimulation activities. Other methods that can help individuals with severe brain injuries regain sensory awareness include electrical stimulation and acupuncture.
How Long Does It Take to Recover from Severe Brain Injury?
Recovering from a severe brain injury can take a significant amount of time and effort. While some patients do progress quite quickly, most people will require months to years of consistent rehabilitation.
In general, the vast majority of TBI recovery occurs within the first two years. For example, according to statistics gathered from the TBI Model System Program, at two years post-injury:
- 70% of severe TBI patients live independently full time.
- Over 90% live in private residences.
- 50% of patients learn how to drive after brain injury, though they may still have restrictions on driving at night or for long distances.
- 30% have a full-time job.
However, it’s important to note that severe TBI recovery does not end after two years. Many individuals continue to improve at five or even ten years post-injury. Therefore, if you have not made the progress you wanted after two years, do not give up hope. The brain never runs out of neuroplasticity, which means there’s always potential to improve.
Severe Brain Injury: Key Points
A severe brain injury is a serious medical condition that can significantly affect one’s quality of life. Depending on the location and severity of your TBI, a wide range of motor, sensory, and cognitive functions can be affected. Luckily, with the right interventions and enough persistence, there is potential to treat these effects and significantly improve your quality of life after TBI.
To inspire you even further, discover 5 inspiring severe brain injury recovery stories. We hope this article encourages you to never lose hope during your recovery journey.