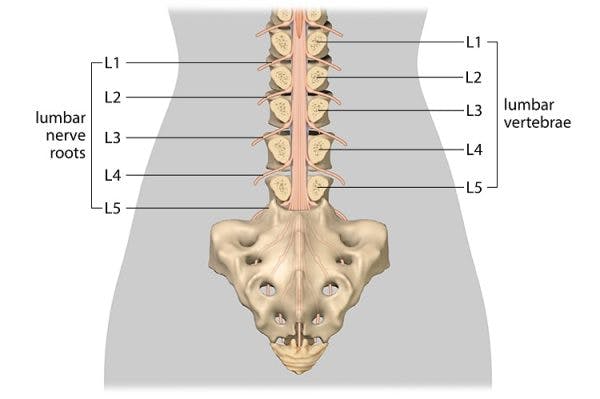
When a spinal cord injury (SCI) is caused by external forces, such as a car accident or fall, it is called a traumatic spinal cord injury. Often, these external forces fracture or shift the vertebrae in the spine, causing compression of the spinal cord. This can potentially lead to permanent damage; however, it is possible for individuals to recover functions affected by SCI and improve their quality of life.
To help you understand what a traumatic spinal cord injury is, this article will discuss its:
Causes of Traumatic Spinal Cord Injury
Spinal cord injuries can be traumatic or non-traumatic. When a spinal cord injury is non-traumatic, it means it is caused by internal complications such as spinal stenosis, tumors, infections, and herniated discs. In contrast, traumatic spinal cord injuries are caused by external forces.
Common causes of traumatic spinal cord injuries include:
- Motor vehicle accidents
- Falls
- Sports accidents
- Acts of violence
These external forces strike the spinal column, often causing the vertebrae to compress the spinal cord. Because the spinal cord is a bundle of nerves that transmits sensory and motor information between your brain and body, individuals may experience a wide range of secondary effects.
Secondary Effects of Traumatic Spinal Cord Injury
Depending on the location and severity of a traumatic spinal cord injury, individuals may experience various secondary effects.
Common effects of traumatic spinal cord injuries include:
- Weakness/paralysis occurs when motor signals from the brain cannot travel through the site of injury to reach the muscles. As a result, individuals may struggle with controlling their movements and balance.
- Weakened/complete loss of sensation occurs when sensory signals from the body cannot travel through the site of injury to be processed by the brain. As a result, individuals may not be able to feel tactile stimulation below their level of injury.
- Bowel, bladder, and sexual dysfunction occur because signals from the brain cannot reach the bowel or bladder muscles, or sexual organs.
- Autonomic dysreflexia is characterized by a hyperactive autonomic response when areas below your level of injury are stimulated. The autonomic nervous system is responsible for regulating involuntary body functions. As a result, individuals may experience a spike in blood pressure, increased pulse, excessive sweating, changes in body temperature, and feelings of panic.
- Pressure ulcers refer to skin breakdown caused by prolonged pressure on one area of the body. After an SCI, individuals may lose sensation and not feel the urge to shift positions. Consequently, they may remain in the same position for extended periods, which disrupts circulation, causes tissue death, and skin breakdown.
- Breathing difficulties may occur after SCIs that disrupt connections to major breathing muscles such as the diaphragm, intercostal muscles (the muscles in between your ribs), and abdominals.
- Changes in body composition occur when individuals with weakness/paralysis significantly decrease their physical activity levels/ do not adjust their diets. This may lead to muscle atrophy and decreased bone density, which can increase one’s risk of falls.
- Spasticity describes involuntary muscle contractions caused by disrupted communication between the brain and muscles. As a result, individuals with spasticity may experience stiff movements, spasms, and restricted range of motion.
Fortunately, with the right support and treatment interventions, many individuals are able to overcome these secondary complications and significantly improve their quality of life.
Is it Possible to Recover from Traumatic Spinal Cord Injury?
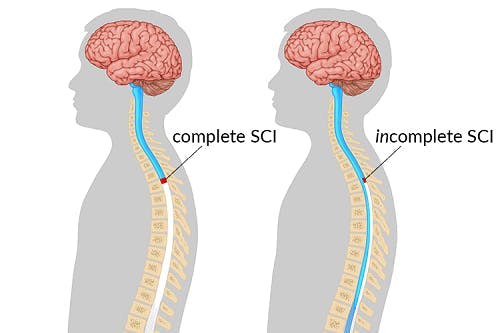
Knowing the severity of your traumatic spinal cord injury can help you understand how likely it is to achieve a full recovery. One way to classify the severity of a spinal cord injury is to determine whether it is complete or incomplete.
A complete spinal cord injury refers to damage the transects the entire spinal cord. As a result, all connections between the brain and areas below the level of injury are affected. Because damaged neurons in the spinal cord are unable to heal themselves, no motor control or sensation will exist below the level of injury.
In contrast, an incomplete spinal cord injury refers to damage that only partially transects the spinal cord. As a result, some connections between the brain and areas below the level of injury may be unaffected or spared. This allows for some motor control and sensation to exist below the level of injury.
Spared connections in the nervous system play a major role in predicting recovery outlook after traumatic spinal cord injury because they are capable of neuroplasticity. Neuroplasticity refers to the central nervous system’s ability to reorganize its neural circuitry and make adaptive changes based on the movements you regularly perform.
It allows for functions affected by spinal cord injury to be reorganized to unaffected regions and improved through massed practice. In other words, it means that there is potential for individuals to recover movement after traumatic SCI.
Even after your spinal cord injury transitions into a chronic phase and recovery occurs at a slower rate, improvements are still possible many years after the initial injury. In the following section, we’ll discuss various interventions that can help individuals recover functions affected by SCI.
Traumatic Spinal Cord Injury Treatment
A traumatic spinal cord injury is a medical emergency that requires proper treatment. As a result, immediate medical attention is necessary to stabilize the spinal cord and minimize secondary damage.
Early treatment goals for traumatic spinal cord injury include decreasing inflammation around the spinal cord, increasing blood flow, and preventing the progression of secondary processes. After stabilizing the injury, treatment goals focus more on restoring or rehabilitating movement and sensation.
Every spinal cord injury and recovery process is unique. Therefore, a personalized rehabilitation regimen that focuses on the individual’s specific complications is ideal.
Rehabilitation after traumatic SCI may consist of:
Physical Therapy
Physical therapy focuses on helping individuals regain motor control and maximize their mobility after traumatic spinal cord injury. This is primarily done by guiding individuals through targeted exercises in a safe and effective way.
Consistently performing exercises that target affected muscle groups stimulates the spinal cord and reinforces demand for those functions. This encourages neuroplasticity in the spinal cord to reestablish and strengthen the connection between the brain and those muscles.
Occupational Therapy
Occupational therapy focuses on helping individuals develop their functional independence after traumatic spinal cord injury.
Due to weakness/paralysis, individuals may need to learn new ways to perform everyday activities such as grooming, feeding, and performing transfers. An occupational therapist can teach them safe and effective adaptive techniques to help them become as independent as possible.
Additionally, an occupational therapist can guide individuals through the process of returning to school or work and understanding their disability rights.
Speech Therapy
If communication or oral motor skills are affected by a traumatic spinal cord injury, doctors may recommend working with a speech-language pathologist. For example, a speech-language pathologist may have you practice oral skills to strengthen the muscles around the face to reduce the risk of choking that can cause further complications.
Orthotics
Orthotic devices such as braces or splints provide musculoskeletal support. After a traumatic spinal cord injury, individuals may struggle with abnormal tone or spasticity in the limbs. This can pull the body into abnormal postures. Wearing orthotics helps promote optimal body alignment and combats spastic muscles from further tightening.
Interestingly, many individuals with SCI learn to take advantage of increased muscle tone by using it to assist with transfers. Orthotics can also help provide extra support to ensure that limbs are stable and won’t collapse with increased pressure.
Medications
Depending on what types of secondary effects are experienced, a wide range of medications may be recommended. For example, individuals with severe spasticity may be recommended Botox injections or muscle relaxants to temporarily relieve high muscle tone. In contrast, those experiencing pain may be recommended different types of pain relievers.
Traumatic Spinal Cord Injury: Key Points
A traumatic spinal cord injury is caused by an external force striking your spinal column and compressing the spinal cord. This most often leads to weakness/paralysis and loss of sensation; however, it can also lead to a wide range of additional complications.
If you have an incomplete spinal cord injury, there is often hope to recover affected functions. However, that is not to say that individuals with complete spinal cord injuries cannot find ways to be functional and improve their quality of life.
By participating in rehabilitative therapies, specialists can help you maximize your mobility and functional independence. We hope this article helped you understand what to expect after a traumatic spinal cord injury and how to promote recovery.