Individuals with cerebral palsy often have an increased risk of hip dislocation due to high muscle tone in the legs. High muscle tone, or hypertonia, can place excess strain on the joints, including the hips. As a result, hip problems may develop, which may lead to pain, asymmetrical growth, and difficulties with balance. Fortunately, there are ways to detect hip problems early and treat them before further complications develop.
To help you understand the association between hip dislocation and cerebral palsy, this article will discuss:
- Anatomy of the hips
- What causes hip problems in individuals with cerebral palsy?
- Signs of hip dislocation
- Why hip dislocation is more common in children with cerebral palsy
- How to treat hip dislocation in individuals with cerebral palsy
The Anatomy of the Hips
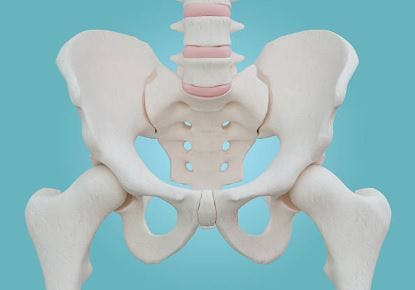
Before we discuss why individuals with cerebral palsy are more likely to experience hip dislocation, let’s review the anatomy of the hips.
The hips are a ball-and-socket joint that allows the leg to move in many different directions (planes). It can move:
- forward and back (like during walking)
- side to side (like when walking sideways or crossing the legs)
- rotate inward and outward (pigeon toeing or out-toeing)
With more movement planes comes less stability. For comparison, the knee joint can only move in one plane (bending and straightening), making it a much more stable joint. As a result, it is much easier for the hip joint to be displaced or even dislocated than a less mobile (and consequently more stable) joint, such as the knee.
Common hip problems that an individual with cerebral palsy may experience include:
- Dysplasia describes when the ball and socket aren’t a perfect fit
- Subluxation describes when the ball is displaced and not secured but still within the socket
- Dislocation describes when the ball moves out of the socket altogether
Now that you understand why the hips are more susceptible to displacement, the next section will discuss what causes hip problems in individuals with cerebral palsy.
What Causes Hip Problems in Individuals with Cerebral Palsy?
Hip problems in individuals with cerebral palsy are most frequently attributed to spasticity in the legs. Spasticity refers to involuntary and prolonged muscle contractions caused by neurological damage. If not properly managed, spasticity can progress, which can cause the muscles to further tighten, limit range of motion, and increase strain on joints such as the hips.
The risk of hip displacement progressing to hip dislocation in children with cerebral palsy is about 15-20%. Additionally, it’s suggested that there is a linear relationship between hip dislocation and a child’s Gross Motor Function Classification System (GMFCS) level. In other words, the more severe your child’s cerebral palsy is, the more likely they are to experience hip dislocation.
To prevent the progression of hip complications, early identification and appropriate treatment of the underlying spasticity is essential. The following section will discuss common signs of hip dislocation as well as the risks associated with untreated hip problems.
Signs of Hip Dislocation
Hip dislocation can start developing in children with cerebral palsy as early as age 2 but is most frequent between ages 3-5. Because the risk of hip dislocation in early childhood is so high, identifying the signs of hip problems as early as possible and appropriately managing them is critical.
Individuals with hip dislocation may experience:
- Difficulties sitting, standing, or performing transfers
- Hip pain
- Restricted range of motion
- Asymmetrical growth of the legs
- Compromised posture
- Abnormal walking patterns or inability to walk
It is recommended that children with more severe cerebral palsy get a radiograph every 6 months to assess whether the hips are properly aligned and document changes over time. The following section will discuss how age affects the risk of hip dislocation.
Why Hip Dislocation is More Common in Children with Cerebral Palsy Than Adults
Generally, the younger you are, the more cartilage covers the hip socket. Cartilage is a slippery substance that allows the bones to slide against each other.
However, in cases where the ball and socket aren’t a perfect fit, having a lot of cartilage can increase the risk of hip displacement. As a result, hip dislocation is more common in children with cerebral palsy than in adults.
As we get older, the amount of cartilage covering the hip socket decreases from wear and tear. Consequently, the risk of hip dislocation also decreases.
Now that you understand the causes, signs, and risks of hip dislocation in individuals with cerebral palsy, let’s discuss treatment.
Cerebral Palsy Hip Dislocation Treatment

The goal of preventative hip dislocation treatment in individuals with cerebral palsy is to maintain flexibility and alignment of the hips while minimizing pain.
Hip dysplasia may not bother your child for years, which is why so many people put off getting treatment until it starts becoming painful and restricting their ability to perform everyday tasks. The key is to avoid waiting until symptoms become problematic and seek early management to minimize the risk of hip dislocation.
Below, we’ll discuss various interventions that may help individuals manage hip displacement.
Physical Therapy
To minimize the risk of hip dislocation in individuals with cerebral palsy, interventions should focus on treating the underlying spasticity. One of the most effective ways to do so is through participating in intensive physical therapy.
Physical therapy will focus on lengthening tight muscles, strengthening underused muscles, and promoting proper form through exercise and manual techniques.
Lengthening muscles such as the hamstrings, hip flexors, and quadriceps may help relieve strain on the hip joints. Additionally, correcting abnormal movement patterns will help ensure that the femoral head (the ball) remains centered and secure in the hip socket.
By consistently practicing the targeted exercises learned in physical therapy, individuals can promote adaptive changes in the brain (neuroplasticity), which may reduce the impact of spasticity in the legs.
Orthotics
Orthotic devices such as braces and splints help gently stretch spastic muscles and provide the structural support necessary to promote proper bone alignment. They will also restrict unwanted movements caused by spasticity.
Botox
Botox is a nerve blocker that is injected into spastic muscles to temporarily relieve high muscle tone. However, it’s effects tend to wear off within 3-6 months.
To promote long-term spasticity relief, individuals should take advantage of the reduced muscle tone provided by Botox and pursue intensive physical therapy. Great improvements can be made while under the effects of Botox, and these improvements can carry over even once the medication has worn off.
Surgery
Surgical interventions will vary based on the degree of the individual’s hip displacement.
For example, soft tissue lengthening may be recommended to prevent hip dislocation and improve subluxation. This procedure involves manually lengthening tight muscles and tendons to decrease tension on the bones and joints.
In contrast, those with more severe forms of hip dysplasia may require femoral or pelvic osteotomy. This procedure involves cutting, repositioning, and reattaching the bones with rods and screws to ensure more secure alignment of the hip joint.
Cerebral Palsy and Hip Dislocation: Key Points
Because children with cerebral palsy are rapidly growing and often experience spasticity in the legs, they have a greater risk of experiencing hip dislocation. If not properly treated, hip dislocation can cause pain, asymmetrical growth, and affect an individual’s ability to walk. Therefore, early intervention is essential for preventing hip problems from progressing.
We hope this article helped you understand why hip dislocation occurs in individuals with cerebral palsy and the best practices to minimize its impact on your child’s growth and development.










