When a brain injury affects the thalamus, it can lead to sensory and/or cognitive side effects. This article will share symptoms and treatment to help you understand the ways in which thalamus damage can affect your everyday life.
As with all types of TBI, it’s important to work closely with your medical team during recovery.
What is the Thalamus?
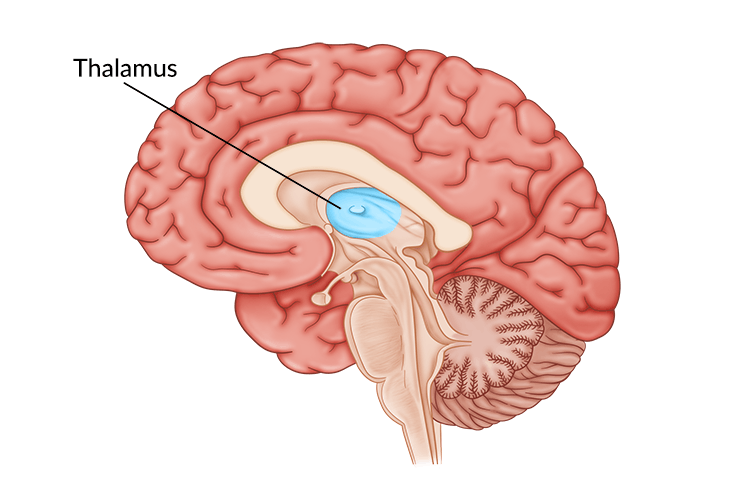
Most neurologists refer to the thalamus as the brain’s relay station. That’s because almost all sensory information must pass through it before moving on to the cerebral cortex.
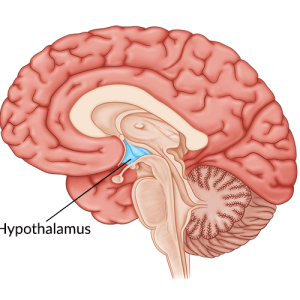
These sensory signals travel up the spinal cord and into the thalamus, which lies just above the brainstem. The thalamus then processes these signals and passes them on to the relevant brain region.
Besides signals from sensory systems, other information travels within the brain itself, which the thalamus also plays a role in. At times, the thalamus even assists with cognitive processes as well, such as memory and emotion.
One of the main processes that the thalamus controls is the regulation of consciousness and sleep. In fact, during sleep, the thalamus actually blocks sensory signals from reaching the rest of the brain. This allows a person to sleep without disturbance.
Finally, the thalamus acts as a bridge between the primary motor cortex and the cerebellum and thus plays a crucial role in muscular movement.
Side Effects of Thalamus Damage After Brain Injury

As you can see, the thalamus contributes to a broad range of critical functions. Therefore, the side effects of thalamus damage can vary from person to person.
Some of the most common side effects of thalamic damage include:
- Sensory issues such as tingling, numbness, hypersensitivity,
- Chronic pain
- Vision loss or light sensitivity
- Motor impairments
- Tremors
- Attention problems
- Memory loss
- Aphasia
- Insomnia
Because the thalamus controls sleep and arousal, severe damage to it can also result in a coma.
Treating Thalamic Brain Injury
Treatment for thalamic damage will revolve around restoring the abilities lost after brain injury. There are many different ways to accomplish this.
The following are some treatments that can help you overcome the effects of damage to the thalamus:
1. Physical Therapy
If your brain injury damaged your thalamus, you might experience problems coordinating movements — a condition called apraxia. For example, you might begin walking with a wide, staggering gait or have trouble reaching for an object.
Since apraxia doesn’t usually affect muscle strength, the best way to treat it is to activate neuroplasticity. You can do this by practicing meaningful movements you want to regain.
For example, if you have trouble eating, you should practice each movement individually before putting them all together. The steps you take might look like this:
- Step 1. Bring hand down to the table
- Step 2. Open fingers
- Step 3. Grasp spoon etc…
It is important to identify ways to make large activities, like eating, into smaller and more manageable tasks to avoid frustration and fatigue. Practicing these skills with multiple repetitions can stimulate neuroplasticity and encourage the brain to recreate new neural connections.
To regain full control of your muscles, it’s crucial to practice even when you are not in a formal rehab setting. Home therapy tools like FitMi can help you stay motivated and achieve the repetitions needed to rewire your brain and improve movement.
2. Sensory Reeducation Exercises

You can also treat sensory issues by rewiring the brain. The best type of therapy to help you accomplish this is sensory reeducation exercises.
Sensory reeducation, also known as sensory retraining, is a form of cognitive-behavioral therapy that teaches the brain how to process sensation again.
Some examples of sensory exercises include:
- Sensory locating. Close your eyes and have someone else place their hand on your arm. Next, point to where you think they touched you. If you get it wrong, have them move your hand to the correct spot. This helps retrain your brain to recognize where they touched you.
- Temperature differentiation. Soak one cloth in cold water and one in hot water. Have someone place the cold cloth on your arm while you close your eyes. Then, switch to the warm cloth. See if you can feel a difference. Alternate back and forth between hot and cold 10 times.
Finally, make sure you practice these exercises every day consistently. This will stimulate your thalamus and help it relearn how to process your senses again.
Want 20 pages of brain injury recovery tips in PDF form? Click here to download our free ebook “15 Things Every TBI Survivor Must Know” (link opens a pop up for uninterrupted reading)
3. Speech and Cognitive Therapy
While thalamus damage primarily causes sensory problems, it can also lead to behavioral and cognitive changes.
For example, many patients with a thalamus injury have incorrect speech patterns and can struggle to find the right words. Others display apathy and memory problems.
To treat these issues, it’s crucial to begin speech therapy as soon as possible. Most speech therapists are familiar with the cognitive effects of brain injury as well. Therefore, they can teach you strategies to improve your memory, language, word-finding skills, and behaviors.
Learn more about speech therapy for brain injury patients »
4. Deep Brain Stimulation

Finally, thalamic damage often leads to tremors. If your tremors are severe, a doctor might recommend deep brain stimulation.
Deep brain stimulation (DBS) is an effective treatment for post-traumatic tremors. DBS uses surgically implanted electrodes to send high-frequency signals to the thalamus. That signal can eliminate tremors.
There is also evidence that thalamic stimulation can enhance cognitive performance after brain injury. This makes it even more helpful for patients with thalamus damage.
With that said, DBS is a surgical intervention with risks and possible side effects, like slurred speech and balance problems. Still, if your symptoms are severely affecting your day-to-day function, it might be worth asking your doctor about it.
Recovering from Damage to the Thalamus
Thalamus damage often leads to sensory and motor deficits. Fortunately, you can treat both of these issues by rewiring your brain.
Because the thalamus has so many different roles though, every injury is different. Therefore, it’s crucial to work with your doctors to find the treatments that best fit your unique needs.
We hope this article helps you better understand thalamus injuries and achieve a full recovery from TBI.