A C1 spinal cord injury refers to a type of cervical spinal cord injury that affects the uppermost region of the spinal cord. As a result, a C1 spinal cord injury can affect motor control and sensation throughout the entire body.
This article will go over everything you need to know about a C1 spinal cord injury (SCI) including:
- The Anatomy of the Spinal Column
- Diagnosing a C1 Spinal Cord Injury
- Effects of a C1 SCI
- Potential Complications
- Recovery Outlook
- Management Techniques
Anatomy of the Spinal Column
The spinal cord is comprised of nervous tissue extending down the back from the base of the brain. It serves to connect the brain with the rest of the body. As such, the spinal cord is essential for transmitting messages regarding movement and sensation between the brain and the rest of the body. When the spinal cord is damaged, messages regarding movement and sensation may be disrupted, resulting in motor and/or sensory impairments.
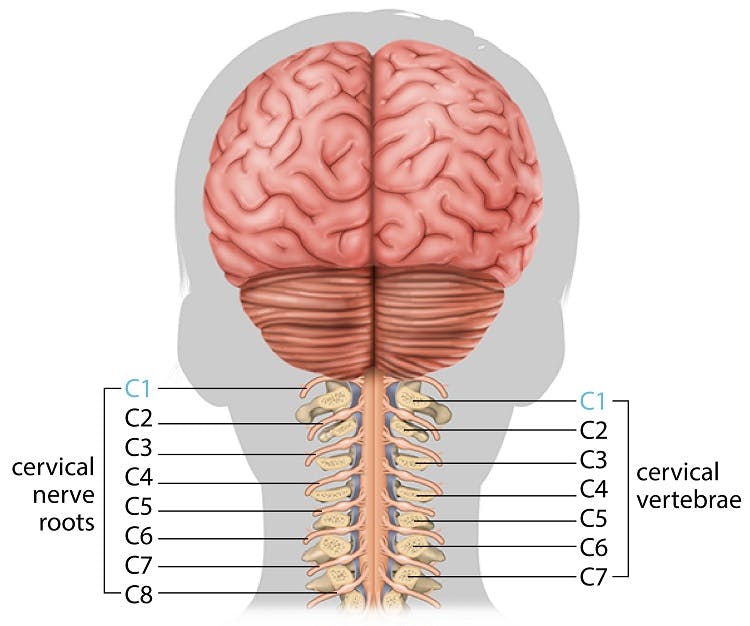
The cervical region of the spinal cord, located in the neck area, is encased within the 7 cervical vertebrae at the top of the spinal column. Pairs of spinal nerves branch off of the spinal cord, exiting the spinal column above their corresponding vertebrae.
The C1 and C2 vertebrae are different from other vertebrae in terms of shape and function. Despite being the smallest vertebrae in the entire spinal column, they form the joints responsible for movement of the head.
The C1 vertebra (also known as the atlas) is the uppermost vertebra of the spinal column. It connects to the base of the skull, forming the atlanto-occipital joint. This joint allows the head to nod up and down.
Underneath the atlas lies the C2 vertebra (also known as the axis). The axis has a small, peg-like projection called the dens. The dens points upwards into the ring-shaped atlas to form the atlanto-axial joint, which allows the head to turn side to side. Because the C1 and C2 vertebrae are so closely aligned, injuries to these vertebrae often occur together. The atlas and axis are crucial because they stabilize the skull, enable neck movement, and protect the spinal cord.
The C1 spinal nerves exit the spinal cord just above the atlas. While all other pairs of spinal nerves have a sensory component that transmits sensory information to the brain and a motor component that allows the brain to tell the muscles to move, the C1 spinal nerves typically have only a motor component.
The C1 spinal nerves, as well as the C2 spinal nerves, are responsible for the muscles involved with nodding the head. However, since the C1 nerves do not have a sensory component, there is not a specific area of sensation associated with the C1 spinal nerves.
After a C1 spinal cord injury, information from the C1 spinal nerves can still be transmitted from the brain to the rest of the body. However, the transmission of all sensory and motor messages below this level may be affected, potentially resulting in a loss of movement and sensation in the neck, arms, legs and trunk.
Diagnosing a C1 Spinal Cord Injury
Because C1 is the uppermost level of the spinal cord, a C1 spinal cord injury can affect motor control and sensation throughout the entire body, with the exception of the face.
This occurs because messages between the brain and areas below the level of injury are unable to be transmitted through damaged areas of the spinal cord.
When an individual sustains a spinal cord injury, a physician will test their sensory and motor functions in accordance with the American Spinal Injury Association (ASIA) Exam. This allows them to determine both the level and severity of the injury.
The level of injury refers to the lowest segment of the spinal cord where motor control and sensation remain intact. In the case of a C1 spinal cord injury, functions associated with the C1 spinal nerves are left intact, but all other sensory and motor functions may be impaired. This is because messages between the brain and body cannot pass through damaged areas of the spinal cord.
However, depending on the severity of the injury, a C1 spinal cord injury may not result in a total loss of motor control and sensation throughout the body.
A complete SCI is the most severe type of spinal cord injury, and refers to spinal cord damage that completely severs the spinal cord. When a complete spinal cord injury occurs, all connections between the brain and areas of the body below the level of injury are cut off, resulting in a loss of all movement and sensation below the level of injury.
In contrast, an incomplete SCI refers to when the spinal cord is only partially damaged at the level of injury. Incomplete spinal cord injuries result in spared neural connections, allowing the brain to still send and receive some messages with areas of the body below the level of injury. Thus, individuals with incomplete spinal cord injuries will have some movement and/or sensation below their level of injury.
While the ASIA exam can help to identify the severity of a spinal cord injury, often a CT scan or MRI is used to more conclusively determine whether the injury is complete or incomplete.
Generally, the milder the spinal cord injury, the more spared neural pathways exist, and the greater the recovery outlook.
Effects of a C1 Spinal Cord Injury
Since a C1 spinal cord injury is the highest level spinal cord injury that can occur, it has the possibility to affect the most functions. Although the effects of a C1 spinal cord injury may vary based on severity, many individuals experience the following:
1. Breathing Difficulties
Without immediate medical attention, C1 spinal cord injuries are typically fatal. The C3-C5 spinal nerves connect to the the main muscle involved with breathing, which is called the diaphragm. Because messages from the brain may not be able to get past the C1 level of the spinal cord, individuals may not be able to breathe.
The main priority when treating someone with a C1 SCI is to stabilize their breathing. Individuals generally require ventilator assistance to restore adequate respiration patterns.
Due to breathing difficulties, individuals may also experience difficulties with projecting their voice when communicating.
2. Loss of Movement and Sensation
A C1 spinal cord injury has the potential to affect movement and sensation throughout the entire body, with the exception of the face. This is because facial movement and sensation is controlled by cranial nerves, which bypass the spinal cord and connect directly to the brain.
Since survivors of a C1 spinal cord injury have such significant sensation and motor deficits, they are typically unable to complete their daily activities independently.
3. Lack of Independence with Daily Activities
As a C1 spinal cord injury can cause paralysis of nearly the entire body, survivors require the full-time assistance of a caregiver to perform activities of daily living like bathing, grooming, feeding, and toileting. While a spouse or other family member may be a survivor’s primary caregiver, many choose to hire a caregiver to help with daily tasks.
4. Bladder and Bowel Dysfunction
Bowel and bladder functions are connected to the lowest segments of the spinal cord. When messages to and from the bowel and bladder cannot pass through damaged portions of the spinal cord, survivors may experience changes to their bowel and bladder functions.
As a result, C1 spinal cord injury survivors may not be able to control their bowel or bladder muscles properly or sense when their bladder or bowels are full. This causes survivors to be susceptible to leaking, accidents, and/or constipation.
To prevent bowel and bladder-related accidents from occurring, individuals with C1 SCIs need to follow a bowel and bladder program.
It is essential for C1 spinal cord injury survivors to properly manage these effects to reduce the risk of complications.
Potential Complications of C1 Spinal Cord Injury
Because a C1 spinal cord injury can significantly change an individual’s motor control and sensation throughout the entire body (with the exception of the face), survivors are likely to experience complications. Understanding potential complications that may arise can help survivors be better prepared to manage them.
1. Body Composition Changes
Since spinal cord injuries at the C1 level can result in paralysis of most of the body, individuals often experience physical changes to the body as a result of limited active movement.
Consequences of reduced physical activity include:
- Decreased bone density
- Muscle atrophy (shrinking)
- Circulation problems
- Slower resting metabolic rate
With these potential complications, individuals may lose a substantial amount of weight in the weeks after their injury due to reduced bone density and muscle mass. Alternatively, some individuals gain weight if they continue to eat similar quantities of food as before their injury, since limited movement reduces the number of calories required.
To minimize significant body composition changes, consider working with a dietician to establish a healthy, nutrient-rich diet.
2. Pressure Sores
If individuals lose sensation after a C1 SCI, they likely won’t feel uncomfortable when sitting or lying in the same position for prolonged periods. However, failure to frequently change positions places excessive pressure on certain parts of the skin, usually in bony areas. This can cut off blood flow and cause the skin to break down. Areas of skin breakdown due to prolonged pressure are known as pressure sores or pressure ulcers.
To prevent pressure sores from developing, change positions every two hours when lying in bed or every half hour when sitting in a wheelchair.
3. Autonomic Dysreflexia
Autonomic dysreflexia is a potentially life-threatening condition characterized by a spike in blood pressure due to stimulation below the level of injury. The most common triggers of autonomic dysreflexia are a full bladder, distended bowels/constipation, tight clothes, skin irritations, and extreme temperatures.
Other symptoms of autonomic dysreflexia include a severe headache, sweating, and shortness of breath.
Limiting exposure to triggers is often the best way to avoid autonomic dysreflexia.
While it is possible to experience serious complications following a C1 spinal cord injury, it is also possible for some to experience great functional improvements through rehabilitation.
C1 Spinal Cord Injury Recovery Outlook
Depending on the severity of one’s C1 spinal cord injury, the recovery outlook will vary.
Since individuals with incomplete spinal cord injuries have some existing neural connections between the brain and the rest of the body, they often have the greatest potential for functional recovery.
This is because the spinal cord is capable of utilizing neuroplasticity, the central nervous system’s ability to rewire itself. Neuroplasticity allows affected sensory and motor functions to be rewired to healthy areas of the spinal cord. Completing targeted, repetitive exercises and activities is the best way to optimize neuroplasticity for recovering functions following an incomplete spinal cord injury.
As individuals with complete spinal cord injuries do not have any neural connections remaining between the brain and the rest of the body at the level of injury, they are unable to utilize neuroplasticity to recover lost functions. However, they can still learn to live fulfilling lives by focusing on compensatory tactics.
Furthermore, new research is being conducted focused on improving functional abilities following high-level spinal cord injuries. This includes studies on stem cell therapy and epidural stimulation, both of which show promising results in promoting functional improvements following a complete spinal cord injury.
Management Techniques After a C1 Spinal Cord Injury
Pursuing rehabilitation is an excellent way to promote recovery after a C1 spinal cord injury. Rehabilitation may include a combination of restorative techniques and compensatory tactics. Restorative techniques focus on improving affected functions, while compensatory tactics focus on optimizing independence with the survivor’s current abilities.
The following are some of the most common types of rehabilitation following a C1 spinal cord injury:
- Physical therapy focuses on maximizing mobility through targeted exercises, manual therapy, and modalities (such as electrical stimulation). Physical therapists can also help survivors and their caregivers learn to safely perform transfers, such as moving from the wheelchair to the bed. If individuals have sustained an incomplete spinal cord injury, physical therapy can help increase movement and strength below the level of injury. Carrying over exercises learned in therapy through a home program is also essential for recovery, as increased repetitions of exercises maximizes neuroplasticity.
- Occupational therapy is centered on optimizing the survivor’s independence and safety with daily tasks. While occupational therapy may include practicing activities of daily living, such as grooming, dressing, and toileting, more often occupational therapists introduce compensatory tactics to help you become as functional as possible. This can involve learning how to use adaptive tools and equipment, such as an eye-gaze controlled power wheelchair. Occupational therapy can also include caregiver training, recommendations on home modifications, and safety education.
- Speech therapy can help you address respiratory and communication difficulties. Speech therapists may use breathing or coughing exercises, voice projection training, or augmentative and alternative communication (AAC) devices to optimize a survivor’s breathing and communication abilities. Depending on the survivor’s abilities and preferences, speech therapists can recommend various types of AAC devices, from a simple paper chart with words and letters to advanced technological software. These devices can allow individuals to communicate through blinking or through their eye gaze if they are unable to communicate vocally.
- Psychotherapy can help survivors and their families cope with the emotional and psychological outcomes of SCI. A psychotherapist can provide helpful insight and resources. Many survivors and their families also choose to join a virtual or in-person support group to share experiences, discuss challenges, and learn from others in similar circumstances.
Pursuing rehabilitation can allow C1 spinal cord injury survivors to optimize and potentially improve their abilities in order to lead fulfilling, engaged lives.
While all C1 spinal cord injury survivors are different, many are able to independently move through their homes and communities using an eye-gaze controlled power wheelchair. Power wheelchairs can be equipped with an attachment for a gaze controlled communication device, allowing survivors to communicate without assistance.
Survivors typically will require full assistance with all daily tasks, including dressing, bathing, toileting, and eating. However, medical equipment providers can help supply individuals with appropriate devices to make all of these tasks doable within one’s own home.
Individuals with C1 spinal cord injuries can also engage in a variety of hobbies, including reading or playing games online with a gaze controlled device, exploring paved paths, or watching sports events. Some survivors may even choose to return to work.
While daily life after a C1 spinal cord injury may look different, survivors can still have an excellent quality of life.
Understanding C1 Spinal Cord Injury
A C1 spinal cord injury can affect functions throughout the entire body, with the exception of the face. However, depending on the severity of injury, motor impairments and loss of sensation will vary.
C1 SCIs are extremely dangerous and often fatal because they can affect one’s ability to breathe. Therefore, it’s essential to seek immediate medical attention.
Life after a C1 spinal cord injury often requires significant lifestyle changes. With the support of your caregivers, rehabilitation specialists, and loved ones, learning to cope and adapt is possible.